New perspective highlights gap between healthcare spending and access to care, with a focus on system-level solutions
Toronto, Ontario--(Newsfile Corp. - April 22, 2026) - The Poirier Group today outlined a new operational perspective on Canada's healthcare wait times crisis, focusing on practical solutions to improve access to care despite rising healthcare spending. Canada continues to experience record healthcare spending alongside growing wait times and limited access to primary care. Recent data, including findings from the Fraser Institute, confirms what millions of Canadians are experiencing: the median wait time from a GP referral to receiving treatment has hit 30 weeks, underscoring the scale of the healthcare wait times crisis in Canada. In some provinces, the situation is even more severe. It is easy to look at these figures, alongside intermittent emergency room closures and the fact that over six million Canadians still lack access to a family doctor and conclude that this is a resource crisis.
The Poirier Group's perspective focuses on how system inefficiencies, patient flow constraints, and resource allocation challenges can be addressed to improve outcomes without relying solely on increased funding.

To view an enhanced version of this graphic, please visit:
https://images.newsfilecorp.com/files/11628/293588_9b8c384ae46c8b1f_001full.jpg
This is happening while Canadian healthcare spending is at an all-time high, raising serious concerns about the efficiency of the healthcare system. The Canadian Institute for Health Information (CIHI) identifies that total health spending has reached nearly $400 billion, or about $9,626 for every Canadian. Since 2005, healthcare spending has increased by over 200% after inflation, far outpacing population growth.
The Poirier Group's analysis indicates that the current crisis is not driven by a lack of funding, but by a systemic misallocation of healthcare resources. Billions continue to flow into the most expensive, reactive parts of the system - hospitals and acute care - while the very foundation that could prevent system strain remains underfunded: primary and preventative healthcare.
A Canadian Healthcare System Dangerously Out of Balance
Year after year, the majority of Canada's health budget is allocated to three primary areas: hospitals (approximately 26%), drugs (14%), and physician services (14%). This is a system largely designed to react to illness rather than prevent it.
In contrast, only 5.3% of total health spending is allocated to primary care, limiting access across the country. This falls well below the 8.1% average among peer OECD countries. Nations such as the Netherlands and the UK, which have stronger access and outcomes, understand that a robust primary care system is the gatekeeper of a healthy population and a sustainable healthcare model. Canada ranks last among top10 high-income countries for primary care access, with only 26% of Canadians able to get a same, or next-day appointment. This gap represents a structural deficit that directly contributes to system-wide pressures.
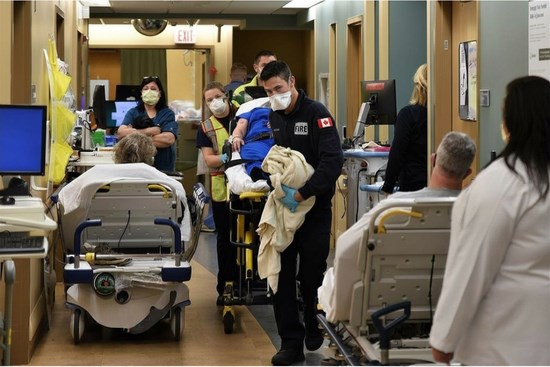
When patients cannot access a family doctor to manage chronic conditions such as diabetes, COPD, or hypertension, those conditions inevitably worsen. As a result, these patients enter the hospital system later, sicker, and at significantly higher cost. This example demonstrates why an underinvestment in primary care access creates a direct and predictable pipeline to hospitals, overwhelming emergency rooms resulting in overcrowding and excessive wait times.
To view an enhanced version of this graphic, please visit:
https://images.newsfilecorp.com/files/11628/293588_9b8c384ae46c8b1f_002full.jpg
Supporting research on acute care spending in a major Canadian hospital reinforces this pattern: high-cost patients were twice as likely to be hospitalized for an "Ambulatory Care Sensitive Condition", an illness that, with proper outpatient care, should not require a hospital stay. In addition, approximately 9% of all inpatient spending for these high-cost patients was for "Alternate Level of Care" days, where individuals remained in costly hospital beds due to a lack of appropriate community or long-term care options.
The result is a system that consistently pays the highest possible cost for reactive care for what could have been preventable outcomes.
"While the gap between spending and access is widely recognized, the path forward is less understood," said Dale Schattenkirk. "Improving patient flow, strengthening primary care access, and optimizing how resources are deployed can significantly reduce wait times without requiring additional funding."
Dale Schattenkirk (Author)
(Healthcare Partner, The Poirier Group)
To view an enhanced version of this graphic, please visit:
https://images.newsfilecorp.com/files/11628/293588_9b8c384ae46c8b1f_003full.jpg
How to Fix Canada's Healthcare System - A Practical Path Forward
The evidence is clear: investing in primary and preventative healthcare delivers significant returns. Addressing the current imbalance requires focused operational improvements across the system, including:
- Expanding clinic capacity through the use of AI-enabled record keeping, connected electronic health records, and reduced administrative provincial documentation burdens.
- Implementing the 'Advanced Clinical Access' model, enabling primary care physicians to manage patient panels of up to 1,200 individuals and significantly reduce the number of underserved Canadians.
- Finally, reallocating the 3% shortfall in funding for primary care from acute care to properly support the preventative healthcare advantage model.
Evidence from primary care reform initiatives in Canada supports this approach. Team-based care models in Alberta and Quebec have demonstrated measurable reductions in emergency department utilization. Similarly, preventative health programs have shown that participants required 25% fewer hospital visits and 17% fewer ER visits within the first year, generating near-term savings of up to $677 per person.
Investing in proactive health management isn't a long-term aspiration; it is a near-term solution capable of bending the cost curve and freeing up acute care capacity within 12 to 24 months.
The path forward is clear. Canada can continue to pour resources into an already strained acute care system, where wait times continue to grow and healthcare professionals face increasing levels of burnout. Or make the strategic pivot the system desperately needs. By reallocating funds to build a world-class primary care network, one that emphasizes prevention, chronic disease management, and integrated care teams, the system can shift toward treating people before they become acute care patients. This approach reduces the pressure on hospitals, brings wait times under control, and supports a healthcare system that is not only properly funded, but functional, accessible and sustainable for all Canadians.

To view an enhanced version of this graphic, please visit:
https://images.newsfilecorp.com/files/11628/293588_9b8c384ae46c8b1f_004full.jpg
About The Poirier Group
The Poirier Group is a North American management consulting firm specializing in business transformation and operational excellence. With deep expertise in healthcare, supply chain, advanced technology, and lean change management, TPG helps health systems improve performance, drive lasting change, and equip frontline teams with practical tools and methodologies.
Visit www.thepoiriergroup.com to learn more.
Media Contact:
Tina Forth
Marketing & Communications
The Poirier Group
905 624-5855
tina.forth@thepoiriergroup.com
To view the source version of this press release, please visit https://www.newsfilecorp.com/release/293588






